NEW
DNA DENTAL DALLAS IS REBRANDING TO REDEFINE DENTAL AESTHETIC AND WELLNESS CENTER
DNA DENTAL DALLAS IS REBRANDING TO REDEFINE DENTAL
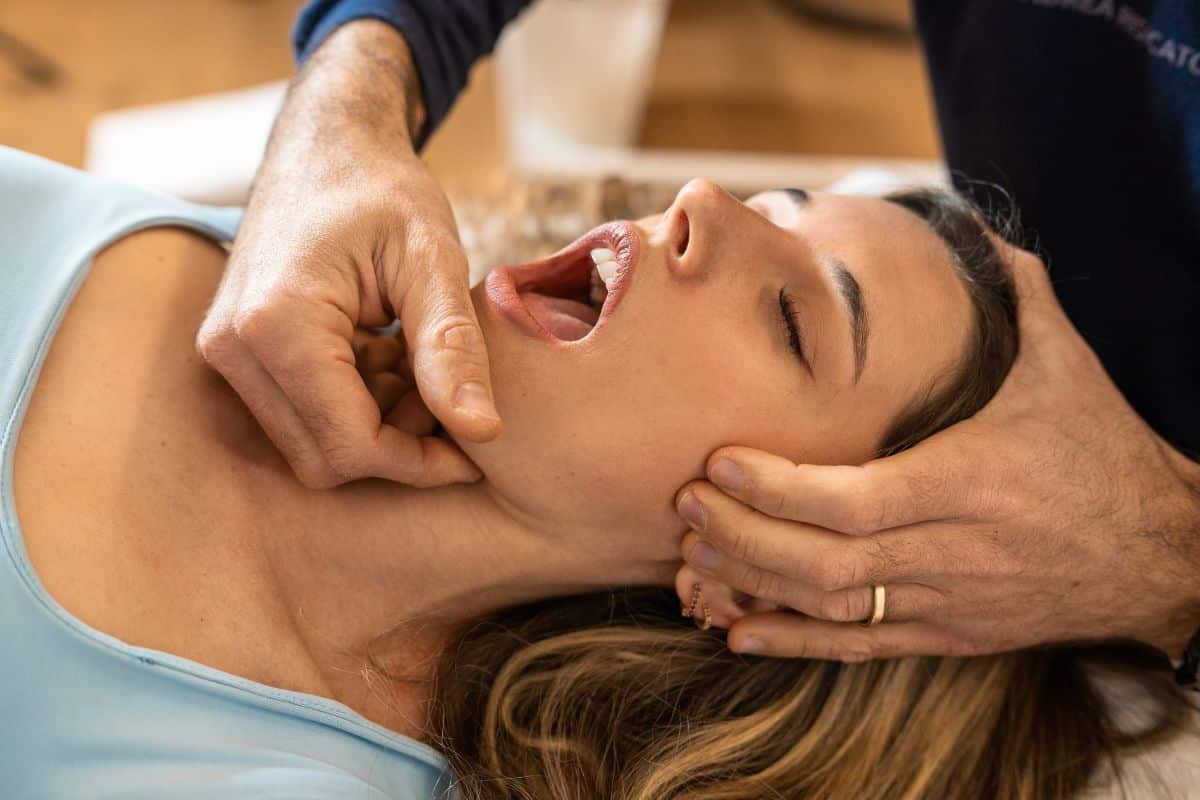
I inject Botox into masseters regularly. It's an effective tool for specific TMJ cases. What I won't do is let a patient walk in expecting Botox to be the whole answer, because for most TMJ problems, it isn't. This post is an honest look at where Botox fits, where it doesn't, and what a full TMJ treatment plan at Redefine Dental actually looks like.
Botox injected into the masseter (the large chewing muscle along your jawline) and sometimes the temporalis (the muscle at your temples) reduces the force of clenching and grinding. For patients whose TMJ pain is primarily driven by overactive jaw muscles, it provides real relief, usually within 1 to 2 weeks, lasting 3 to 4 months. For patients whose TMJ pain is driven by joint inflammation, disc displacement, bite misalignment, or poor sleep posture, Botox alone will not solve the underlying problem. It may mask it, which can delay appropriate treatment. A proper TMJ workup determines which category you're in.
If you've searched "Botox for TMJ Dallas" recently, you've seen a lot of practices advertise Botox as a TMJ cure or as the first thing to try. That framing is incomplete.
TMJ disorders are a category, not a single condition. The temporomandibular joint is a complex structure, and the patterns of pain, clicking, limited opening, and jaw fatigue that patients experience can come from very different underlying causes. A few of them are amenable to Botox. Others aren't. A few actively get worse if masked without addressing the root cause.
So when a patient calls asking about Botox for jaw pain, my first question isn't "when can we schedule the injection." It's "what's actually causing your pain, and have we established that before anyone injects anything."
I tend to sort TMJ cases into three rough categories. Each one has a different role for Botox.
These patients have:
For this category, Botox in the masseters reduces the force of clenching. The muscle is still functional (you can still chew normally), but the peak force it can generate is reduced. That's enough to break the cycle for many patients.
Relief usually starts within a week. Most patients report meaningful improvement within 10 to 14 days. The lower face shape slimming (for patients whose masseters had hypertrophied from years of clenching) is a cosmetic benefit that comes alongside the functional one.
But, and this is important, this is still only part of a plan. For Category 1 patients, I also recommend:
Botox is a meaningful part of the plan for these patients. It's not the entire plan.
These patients have:
For these patients, the root cause is usually at the joint (disc displacement, joint inflammation, degenerative changes in the joint surface). Botox in the masseter can reduce secondary muscle tension, which helps, but it doesn't address the joint issue itself.
For Category 2, the primary treatment is usually:
Botox for these patients is an add-on, not the primary tool.
This is the category that gets missed most often. A significant percentage of TMJ patients have underlying sleep issues (mild sleep apnea, upper airway resistance, or disrupted sleep architecture) that cause them to clench at night as an unconscious response to airway narrowing.
For these patients, treating the clenching with Botox without addressing the airway issue can make the underlying problem worse over time. The Botox reduces the symptom (clenching) without fixing what's causing it.
For Category 3 patients, the appropriate first step is a sleep evaluation, not a Botox injection. We may refer out for a home sleep study. Once the airway issue is understood and addressed (with a or CPAP or other appropriate treatment), the clenching often resolves on its own. In some cases, a Botox treatment in parallel provides additional short-term relief, but the root cause is the airway.
A first TMJ appointment at Redefine Dental is typically 45 to 60 minutes and includes:
That full picture is what determines whether Botox is a good tool for your specific case, and if so, what else needs to sit alongside it.
For patients where Botox makes sense, here's what a typical treatment looks like:
Some dentists and some med-spas will inject Botox into masseters for essentially any patient complaining of jaw pain, as a quick intervention. I don't operate that way, and here's why.
For Category 1 patients, I agree Botox belongs in the plan. But I won't inject unless we've also established a plan for the underlying clenching cause (night guard, bite evaluation, stress or sleep assessment). Injecting Botox without addressing the root habit is giving someone a 3-month reprieve, not a fix.
For Category 2 patients, I believe Botox is secondary to joint-specific treatment. I won't refuse to inject if a patient really wants it, but I'll make sure they understand it's addressing a symptom, not the underlying joint issue.
For Category 3 patients, I won't lead with Botox at all. The airway issue comes first, and in many cases, the need for Botox disappears once the airway is addressed.
This is a slower process than "come in, get the shot, feel better in two weeks." Some patients don't want the slower process and go elsewhere. That's their choice. But the patients who stay for the full workup consistently report better long-term outcomes, because we're treating the actual cause of their pain, not just the muscle it's expressing through.
If you're in Dallas and looking at Botox for jaw pain, the right question to ask any provider isn't "will you do it." It's "what's causing my pain, and what else besides Botox do you think I need." If the answer is just Botox, find a second opinion. If the answer is a comprehensive plan with Botox as one part, you're in the right place.
